MELANOMA is a type of skin cancer that can be life-threatening if not detected and treated early. As a GP, it is essential to be able to identify the signs and symptoms of melanoma and refer patients for further investigation and treatment. However, diagnosing melanoma can be challenging, and there are several pitfalls that GPs need to be aware of.
Misdiagnosis as benign skin lesions
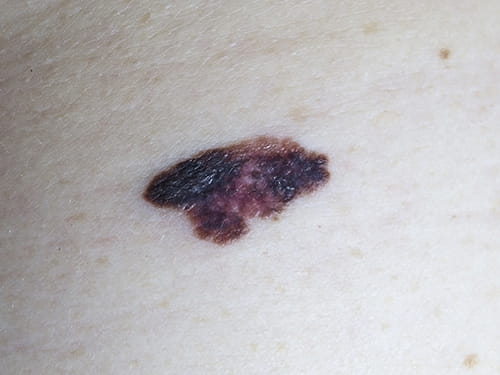
One of the most significant pitfalls in diagnosing melanoma is misdiagnosis as benign skin lesions. Most people have multiple moles, seborrheic keratoses and lentigines, and the vast majority are harmless. Melanomas can often present as a new or changing lesion, and it is important not to dismiss these as benign without proper investigation.
GPs should consider using the ABCDE rule, with the key examination features of melanoma being:
- Asymmetry
- irregular Borders
- multiple Colours
- large Diameter (greater than 6mm)
- Evolving lesion.
If a mole displays any of these characteristics, it may be an indication of melanoma.
Inadequate documentation
Inadequate documentation can be a significant pitfall in diagnosing melanoma. Accurate documentation is essential for effective communication between GPs, specialists and other healthcare professionals involved in the patient's care. Inadequate documentation can lead to delays in diagnosis and treatment, as well as increased risk of medical errors with medico-legal consequences.
When examining a skin lesion, a GP should document a thorough description of the lesion, including its location, size, colour and texture. They should also note any associated symptoms, such as itching, bleeding or pain. It is important to document the patient's medical history, including any previous skin lesions, family history of skin cancer, and any relevant risk factors.
If a dermoscope is used, the GP should document the findings, including any suspicious features. Relevant images or photographs of skin lesions can be stored in the clinical records with the patient’s consent and can act as a future reference for comparison or can be attached to a referral.
Finally, the GP should include a clear plan of action, such as referral for further investigation or follow-up, and provide the patient with appropriate information and advice, including safety-netting in the event of further changes if no immediate action is to be taken.
False sense of security
GPs may have a false sense of security when it comes to diagnosing melanomas, as skin cancer is often thought of as a disease of older individuals or those with significant sun exposure. However, melanoma can affect anyone, regardless of age, skin type or sun exposure history. Additionally, melanoma can occur in areas of the body that are not typically exposed to the sun, such as the scalp, feet, nails and genitals.
Overreliance on dermoscopy
Dermoscopy is a useful tool for evaluating skin lesions and can help GPs distinguish between benign and malignant lesions. Dermoscopy requires training and expertise, and even with its use, some melanomas are missed. GPs should therefore not rely solely on dermoscopy and should also consider the patient's history, clinical examination and any relevant risk factors when assessing a skin lesion.
Lack of follow-up
Another common pitfall in diagnosing melanoma is a lack of follow-up. If a GP detects a suspicious lesion, it is essential to refer the patient for further investigation and follow-up. However, some patients may fail to attend follow-up appointments or may delay seeking further investigation. GPs should ensure that patients understand the importance of timely follow-up and provide clear instructions for follow-up appointments and investigations.
The NICE guidelines on suspected cancer recognition and referral also recommend that GPs provide patients with clear information about symptoms to look out for and when to seek further medical attention. GPs should also have systems in place to ensure that patients who fail to attend follow-up appointments are contacted and encouraged to reschedule.
Failure to consider the possibility of metastasis
Melanoma can metastasise to other parts of the body, including the lymph nodes, lungs, liver and brain. When diagnosing melanoma, GPs should consider the possibility of metastasis and investigate accordingly. Symptoms such as persistent cough, shortness of breath, or unexplained weight loss should raise suspicion of metastasis and prompt further investigation. The NICE guidelines recommend that GPs consider referral for suspected metastatic melanoma if there are symptoms or signs suggestive of metastasis, such as lymphadenopathy, respiratory symptoms or neurological symptoms.
Conclusion
Melanoma is a challenging cancer to diagnose. To avoid the pitfalls, GPs should use tools such as the ABCDE rule, the two-week wait cancer referral pathway and NICE guidelines on suspected cancer recognition and referral. Practices should also provide clear information to patients about the importance of follow-up and have systems in place to ensure that patients attend follow-up appointments. Accurate documentation is also essential for effective communication between healthcare professionals involved in the patient's care.
By being aware of the pitfalls and taking appropriate measures to avoid them, GPs can help to ensure that patients with melanoma are diagnosed and treated early, increasing their chances of a good outcome
References
- Skin cancers – recognition and referral. NICE Clinical Knowledge Summary (CKS) February 2021
- The two-week wait skin cancer pathway. BAD, NHS 4 April 2022, Version 1.
- Clinical ABCDE rule for early melanoma detection. EJD November 2021, Volume 31, Issue 6
This page was correct at the time of publication. Any guidance is intended as general guidance for members only. If you are a member and need specific advice relating to your own circumstances, please contact one of our advisers.
Read more from this issue of Insight Primary

Save this article
Save this article to a list of favourite articles which members can access in their account.
Save to library