These case summaries are based on MDDUS files and are published here to highlight commons pitfalls and encourage proactive risk management. Details have been changed to maintain confidentiality.
 BACKGROUND
BACKGROUND
A dental practice receives a letter from the NHS in regard to a complaint lodged by a patient – Mrs J – who underwent a tooth extraction. She presented at the surgery as an emergency appointment complaining of pain in an upper left first premolar. The dentist – Dr K – undertook an examination and found a large restoration in the tooth, which was mobile and affected by recession extending to the apex.
Both the gum and tooth were extremely tender with pus exuding from the margins. A radiograph showed extensive decay and Dr K recommended extraction.
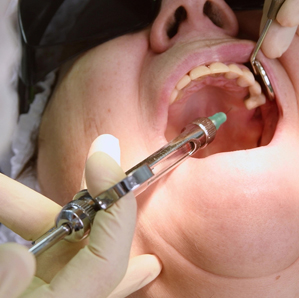
Mrs J consented to the procedure. Three injections were required and Dr K used a topical anaesthetic as Mrs J said she had a “low pain threshold”. She tolerated the first two injections well but the third was to the hard palate and Mrs J gripped the chair rests and cried out. Dr K carried on with the extraction without further incident.
In her complaint Mrs J claims that she found the third injection “excruciating” and that she had to grip the dentist chair to stop herself batting away Dr K’s hand. She questions why he carried on with the procedure without comment or apology when she was “clearly traumatised”.
Mrs J also questions why Dr K provided no warning in regard to the hard palate injection, particularly when she had mentioned her low pain threshold. She demands an apology and reassurance that no other patient will have to endure such an experience.
Dr K contacts MDDUS for assistance in responding to the complaint.
ANALYSIS/OUTCOME
Dr K drafts a letter of response, which is reviewed by an MDDUS adviser. He first expresses regret that Mrs J is unhappy with the care she received at the surgery. He also offers an apology for not warning her that the third injection might be painful even with topical anaesthetic – albeit lasting only a few seconds. In addition, Dr K states that he is sorry for not recognising her level of distress and being more sympathetic – but that there was nothing else he could have done to make the injection more comfortable.
Dr K includes that he has reflected on how the care was provided and will better consider his approach in similar circumstances.
In closing the letter, Dr K states that if Mrs J is unhappy with his response she can forward her complaint to the ombudsman for independent review. Contact details are provided.
Mrs J contacts the practice upon receipt of the letter, stating she is grateful for Dr K’s letter and accepts his apology. She now considers the matter closed and will see him for her next examination appointment.
KEY POINTS
- Explain procedures fully to the patient to ensure informed consent.
- Ensure patients are aware in advance of potential treatment pain/discomfort.
- Be aware that some patients may not be vocal regarding pain/phobias.
This page was correct at the time of publication. Any guidance is intended as general guidance for members only. If you are a member and need specific advice relating to your own circumstances, please contact one of our advisers.
Read more from this issue of Insight Dental

Save this article
Save this article to a list of favourite articles which members can access in their account.
Save to library