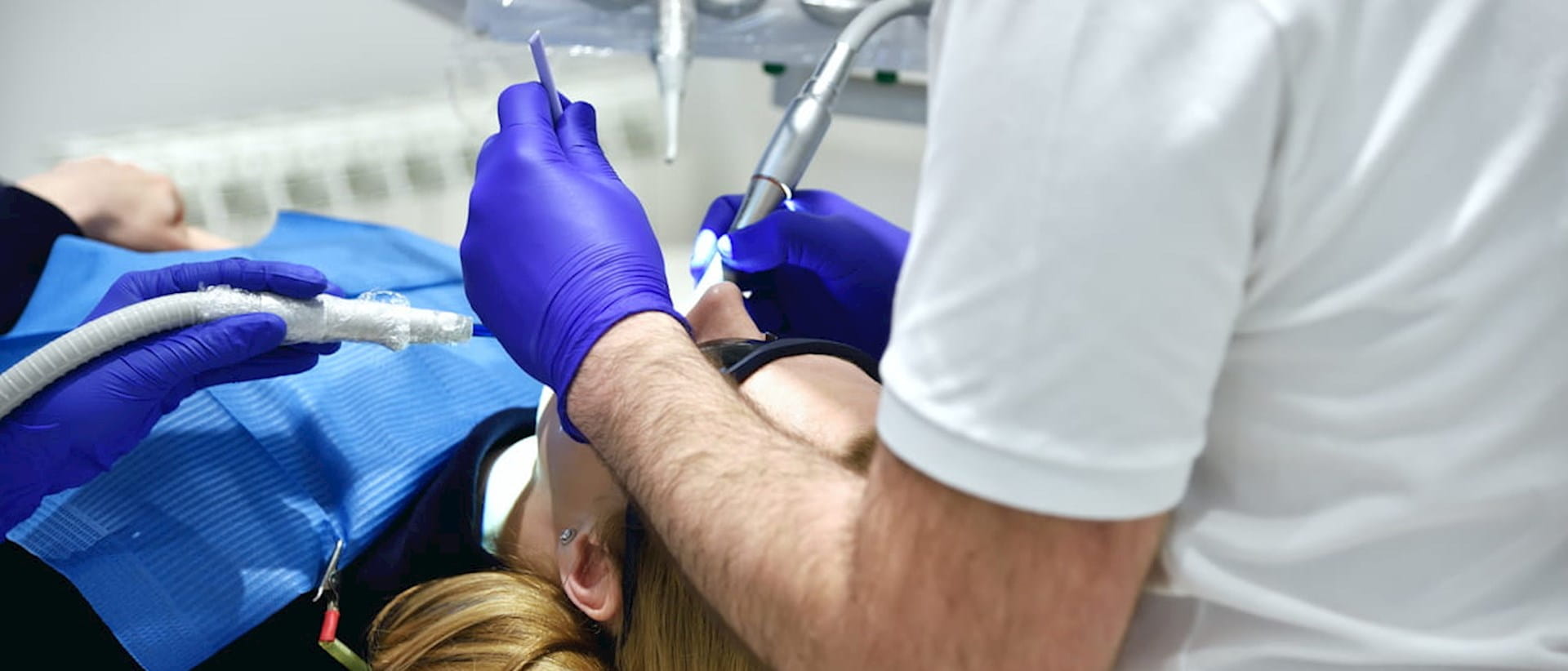
AS dentists and oral surgeons, we are sometimes faced with a procedure that seems “awfully simple” at the outset, but quickly degenerates into something “simply awful”.
This article aims to highlight potential pitfalls in the practice of oral surgery and how we might mitigate them.
Key points include:
- Getting the diagnosis right: take time to conduct a thorough patient history and clinical and radiographic examination.
- Communication with colleagues: this is particularly important where different team members are involved in treatment planning/carrying out clinical treatment.
- Consent: give patients time to understand all available options and clearly document discussions.
- Local anaesthetic: use the correct technique for each patient.
- Aftercare: reviewing patients after surgery can help ensure a positive outcome.
Planning
The best plan we have is the diagnostic pathway. This consists of:
- patient complaint
- history of the presenting complaint
- past medical history
- medication history
- past dental history
- extra oral and intraoral examination
- special investigations.
Note how more than 50 per cent of this “plan” is history-taking.
Clinical examination is also a vital element of the diagnostic pathway and what might seem boring or mundane will get you out of an “incident pit” before you get in.
Assessment of tooth pulp vitality through sensitivity testing and periodontal involvement through percussion are essential, especially when trying to identify the source of pain or infection, along with looking and feeling for signs of swelling – particularly so in the case of potentially life-threatening involvement of facial spaces such as sublingual/submandibular spaces.
Always record the basic signs, such as temperature in the case of spreading infection and mouth opening (which as well as indicating a potentially life-threatening problem will also highlight how much surgical access you will have), and identifying obvious sources of pathology such as carious teeth, draining sinuses and unusual mucosal lesions in high-risk sites.
In oral surgery the most common of special investigations will be radiographs. In my opinion every extraction requires a radiograph (although this is ultimately a matter for each dentist’s own clinical judgement), and every radiograph requires a report. Whilst this can appear tiresome in the context of a busy dental practice, it will help you in making your diagnosis, especially if there were to be an unexpected cause for that mobile tooth you are about to extract.
A radiograph will also assist you in assessing the degree of difficulty of the surgery and therefore whether the surgical task is within your competency, or if you should refer to an appropriate specialist.
You should note the condition of crown, root curvature/number/morphology, bone levels, bone density and proximity to local anatomy such as antral floors and nerve canals/ostia.
It is important to note associated pathology, especially poorly defined bone loss, root resorption or extensive loss of the lamina dura, which may be indicative of more aggressive and worrying osteolytic lesions.
By doing the report you are fulfilling your legal responsibilities as an operator (reporting). You also are now in a better position to communicate to the patient the difficulties that may lie ahead when you are obtaining consent.
Communication
Communication is vital as an oral surgeon. It is particularly so within teams where the person who develops the treatment plan may not be the person who will undertake the treatment.
Communication between dentists, external (and internal) colleagues and patients should be as clear, concise, and contemporaneous as possible. It should be supported with written material for the patient which is easy to read and understand.
Where your practice is to write letters, it does no harm to copy in the patient as another source of written information.
Where possible, I find it is preferable to avoid undertaking surgical treatment on the first visit, as this affords the opportunity to build rapport and manage patient expectations. It also gives time for the patient to internalise the information provided and for you to confirm they have done so at the next visit. Clearly this may not be possible in the context of referral practices currently, but our data would tend to indicate it is a worthwhile consideration.
Consent should also be recorded in the notes, including options provided, their respective appraisal and likely complications. This does not have to be in essay format and will not necessarily avoid legal challenge, but it most certainly will attract adverse attention if not recorded in the event of an outcome which proceeds to litigation. Confirmation that the patient was provided with written information will also be helpful in this instance.
Local anaesthetic
Use the correct LA technique for the job in hand. Your dental history should have revealed any adverse reactions in the past and the patient’s compliance to work under LA.
Do not be tempted to bend needles or use infiltration needles for inferior alveolar blocks. Needle fractures will be a significant disappointment for you and the patient.
Know your maximal dosages and remember how to recognise and manage the more common complications of LA use such as:
- vasovagal syncope
- tachycardia
- delayed trismus
- neuropraxias
- facial palsy
- allergy
- skin blanching.
These are surprisingly rare considering the number of injections given in practice, but it is important not to forget about them and to recognise when they occur and manage appropriately and in a timely fashion.
Complications
The surgical complications that attract most adverse attention are dental extractions and associated problems such as oroantral communications, with failed attempted extractions being the most frequent.
As mentioned above, reaching an incorrect diagnosis and then instituting the incorrect treatment is another common theme.
These are followed in frequency by post-op infections, displaced roots into the antrum and wrong tooth extraction, amongst others.
Honesty when complications occur, effective communication in advance (see above) and early recognition along with prompt corrective action will always be the best approach after prevention. It will certainly help to reduce the risk of a complaint turning into litigation.
Remember, what we tell the patient in advance of surgery is always important in terms of their emotional/mental preparedness, but what we tell them after an adverse event (even a predictable one) can sometimes be seen as an excuse.
Other risk factors
Online consulting
Under-pressure dentists managing large backlogs may see online consultations and the use of non-surgical approaches as a seductive alternative to more traditional approaches, but they are not a panacea. Seeing the patient face–to-face and treating their condition quickly and effectively through appropriate surgical intervention would seem to me to still be the benchmark.
Patient access difficulties
Media reports have commented on the increasing numbers of people who are having difficulties accessing a dentist. There are also those who are going abroad for dental treatment. In these circumstances it is likely that, when patients do eventually get to see their UK dentist, they will require the services of an oral surgeon as dentitions deteriorate beyond the point of restorability. It is also likely that the surgical task will be that more complicated as a consequence of the delay and patients will be that bit less tolerant.
More detailed advice on dental tourism is available in this MDDUS article.
Aftercare
Reviewing patients after a surgical intervention makes sense for many reasons, but busy practices may not always view it as a priority. In my view, it is an effective way to build patient trust. It supports the developing rapport, and it facilitates learning for the practitioner who can see the results of their surgery. It ensures the positive patient outcome anticipated at the outset has been realised. As such it is a “practice builder” and importantly helps the practitioner identify any areas for improvement.
An acceptable compromise might be telephone reviews which would at least help triage cases that do need to be reviewed in the surgery post-operatively.
Provide verbal and written post-operative advice as well as information on who the patient should contact if they experience any difficulties. These are simple ways to help build confidence through knowledge, understanding and trust.
Appropriate and proportionate prescription of analgesia and antibiotics based on published guidelines is also good practice but do not forget these will always be adjuncts to surgical treatment, and using them in combination with surgery will help ensure a positive outcome for ALL involved.
Further information
Oral Surgery journal: Dental negligence: Root cause analysis of an oral surgery expert witness’ experience
This page was correct at the time of publication. Any guidance is intended as general guidance for members only. If you are a member and need specific advice relating to your own circumstances, please contact one of our advisers.
Read more from this issue of Insight Dental

Save this article
Save this article to a list of favourite articles which members can access in their account.
Save to library