
TOOTH wear – encompassing erosion, abrasion and attrition – is usually multifactorial and is increasing in the UK, especially in younger people. There are a myriad of causes, ranging from the much-publicised effects of smoothies, fruit juices and drinks to issues around which there is, perhaps, less awareness, such as stress (resulting in bruxism) and disorders like bulimia.
Just as in every area of oral health and dental care, prevention is preferable to treatment, especially since patients with severe tooth wear may require extensive restorative treatment – but more on that later. Signs and symptoms of tooth wear (see images bottom page), which may or may not be what one would expect for a patient’s specific age (i.e. chronological or pathological), include:
- teeth becoming rounded, smooth and shiny and losing surface characteristics
- incisal edges becoming short and appearing translucent
- cupping forming in the dentine
- cervical lesions which are shallow and rounded
- restorations standing proud of the surrounding tooth tissue (as they tend to be unaffected by erosion).
Patients are often shocked to be told they have a tooth wear problem. This revelation may be especially upsetting for those who have been regular attenders and never been made aware previously, and also for those who have embraced a 'healthy eating' regimen that inadvertently encourages the consumption of acidic – and therefore potentially toothdamaging – foods and drinks. Some of the less well-known culprits include dried fruits, spinach and certain cheeses; all are favourites amongst the health conscious.
It is, therefore, very important that a diagnosis be handled sensitively, and especially so in cases where there is an underlying emotional issue, for example bulimia. Denial and shame are strong features of eating disorders, so emphasise to the patient that you and your team members are there to help. A staged approach, beginning with a nonjudgmental and sympathetic discussion, is ideal.
As with any patient, it is important to share examination findings with them and explain how their signs and symptoms are linked. Aim to make the patient feel comfortable and not intimidated, assure them you have time to talk things through and gently ask questions aimed at encouraging the patient to identify the origin of their oral health problems. Advice rather than treatment features heavily during the initial stage of helping a patient suffering with bulimia.
KNOWING WHEN TO REFER
Of course, it is always important to treat the problem in front of you, but clinicians also need to know their limits. If you do discover that a condition beyond the usual scope of dental practice is contributing to tooth wear, it would be prudent to seek the patient’s permission to liaise with their GP or medical specialist before taking further action. This does not just apply to patients with eating disorders – drug or alcohol addicts, for example, may need extra help too.
Even in general terms, referral to a specialist may be appropriate as tooth wear can be challenging to manage and/or restore. A dentist has a duty of care to refer patients for further advice if they have any concerns about their ability to carry out treatment to an appropriate standard. In addition, if a patient asks for a referral, for example for a second opinion, the dentist must fulfil that request.
When a referral is made, whether through the NHS or privately, it is important to have a process in place to track its progress, and to follow up if a response is not forthcoming from the specialist.
SHARED DECISION-MAKING
Modern dentistry requires any prevention and/or treatment decisions to be made in partnership with an informed patient. To help patients choose how to best move forward in terms of managing their tooth wear (and, indeed, any form of dental treatment), they need to be involved in a number of decision-making steps.
In order to secure valid consent, the dentist must communicate the following effectively (NB: this list is not comprehensive):
- the problem
- any treatment options and their material risks
- costs and the basis for treatment provision (NHS v private)
- benefits and limitations
- the evidence base.
These discussions should be confirmed by, at the very least, a written treatment plan/cost estimate. Dentists also need to understand each patient’s expectations, values, preferences, understanding and any other personal circumstances that may be relevant. At the heart of this process remains patient safety and clinical suitability.
IT’S ALL IN THE NOTES
One fundamental tenet of managing risk in dentistry is keeping high-quality records. Accurate, contemporaneous, legible and up-to-date notes detailing the severity of any tooth wear, indices used, shared decision-making, actions taken and supplementary care are essential additions to the clinical records – always!
Dentists and patients may together choose to simply monitor the tooth wear, and this must be noted in case a claim of supervised neglect is made further down the line. In addition, in the event that a patient cannot or will not make a decision about their own care, it is important to add to the notes that an attempt at shared decisionmaking was attempted and efforts were made to engage the patient. The patient may request treatment which is justifiable but which differs from your recommendations. In these circumstances, it is particularly important to have a clear record of the discussions regarding the relative merits of each option.
This is a significant issue and to cover everything that is important is beyond the scope of this article, so I would recommend accessing the guidance issued by the Faculty of General Dental Practice relating to note taking1.
In addition, it is critical to consider risk assessment2 and to monitor the rate of wear objectively by taking clinical photographs and study casts at regular intervals, perhaps every two to three years for future reference.
It is also important to consider that, although the NHS contract requires the contract holder to keep records for up to two years after a course of treatment has been completed, the Consumer Protection Act 1998 allows claims regarding a “defective product” for up to 10 years. Therefore, both NHS and private records for adults should be kept for a minimum of 11 years following the last entry.
Always remember the adage: "If it’s not written down, it didn’t happen". A dentist who does not have detailed records will be greatly disadvantaged in the event of an accusation that something has gone wrong.
EXCEEDING EXPECTATIONS
Even with the very best of intentions, mistakes do happen – nobody is perfect. In fact, NHS figures suggest that between 1 April 2016 and 31 March 2017, 13,493 complaints were made in England about NHS dentistry, nearly double that for 2015/16, possibly indicating a worrying trend. This may be partly because consumer expectations have risen in recent years, plus experience tells me that patients are more ready to question the care they receive than ever before.
As long as you have managed both your risk and that of your patient in terms of issues such as shared decision making, note taking and appropriate referral, you can rest assured you have provided the best possible approach to managing tooth wear and are in a position to demonstrate exactly that should the regulator come knocking.
Professor Andrew Eder is a specialist in restorative dentistry and prosthodontics and clinical director of the London Tooth Wear Centre, a specialist referral practice in central London. He is also emeritus professor at the UCL Eastman Dental Institute. For further information on the work of the London Tooth Wear Centre go to www.toothwear.co.uk
REFERENCES
- Clinical Examination and Record-Keeping: Good Practice Guidelines www. fgdp.org.uk; May 2016
- Worn’ing: Tooth Wear Ahead. Slater L, Eder A. and Wilson, N Prim Dent J. 2016; 5(3): 38-42
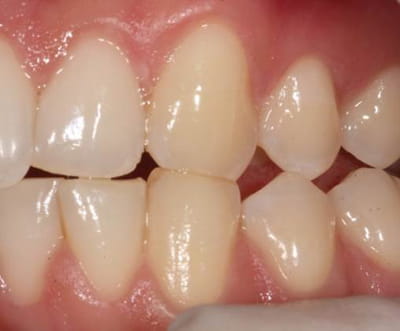
Pathological attritional wear of the canines in an 18 year old (top).
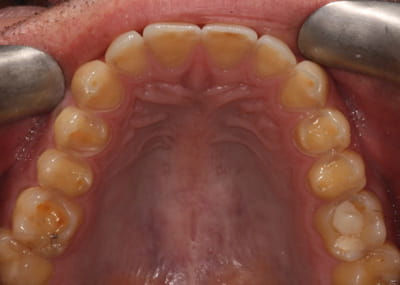
Palatal erosion and enamel loss in a 44 year old (middle).
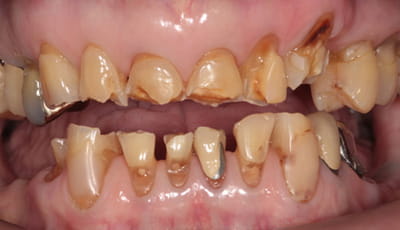
Tooth wear and missing teeth in an 80 year old (bottom).
All clinical images courtesy of Professor Andrew Eder
This page was correct at the time of publication. Any guidance is intended as general guidance for members only. If you are a member and need specific advice relating to your own circumstances, please contact one of our advisers.
Read more from this issue of Insight

Save this article
Save this article to a list of favourite articles which members can access in their account.
Save to library